
Institute of Neonatology, Belgrade, Serbia
 latinica |
 ћирилица |
 english |
 |
Institute of Neonatology, Belgrade, Serbia |
|
First Serbian Human Milk BankFor many years Institute of Neonatology had collected surplus human milk from mothers that were hospitalized alongside their infants and used it to feed other newborns. Nevertheless this activity was limited because of the lack of adequate equipment to form a fully functional human milk bank. Recently with the help generous donations from local authorities and many companies and individuals the most modern equipment has been acquired, and human milk bank has been set in operation in March 2010. Now it is possible to collect, analyze, pasteurize, deeply freeze and store mother’s milk, and than to use it for feeding newborns, or to precisely fortify the milk before using it. This is the first such milk bank in Serbia and also in the region of Southeast Europe. http://www.bankamleka.rs/ Dr Slavica Simić On 14 May 2009 the Committee for evaluation of health technologies of Serbian Ministry of Health has approved the implementation of Human Milk Bank in Department for nursing mothers in Institute for neonatology. In October 2010 Human Milk Bank of the Institute of Neonatology in Belgrade (Serbia) was recognized as a member of European Milk Banking Association (EMBA). History At the beginning of 20th century all infants were breast fed (by mothers or wet nurses). At the beginning of 21st century we are facing the circumstances of having to put great effort in reaffirmation of this biological activity. New technologies in 20th century such as pasteurization and freezing enabled the first human milk banks to be formed. One such bank has been formed in Vienna in the year 1909. The first guidelines were published by HMBANA in 1990. Human milk banks are non profit organizations for collection, analyzing, processing, storing and distributing donor breast milk in order to fulfill the particular medical needs of the recipients. They operate under clearly defined standards (HMBANA, UKAMB). Importance of milk banks for adequate nutrition of newborns More than 1.5 million children die every year due to inadequate nutrition. In the first 2 to 3 years of life adequate feeding is crucial because it is a critical period for formation of metabolic functions, growth and development. If influence of optimal nutrition in that period is not utilized, a "window of opportunity" might get permanently lost. Human milk has all the necessary nutriments for fetal and postnatal development. It is the exclusive food for term infants during the first 6 months of life, and can be used until 2 years of age in combination with complementary non-milk food. Low birth weight newborns (< 2500 g) - LBW 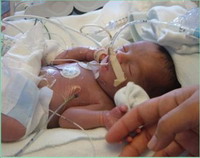 Every year 20.6 million children of low birth weight are born. These
children are in special risk for postnatal growth restriction,
infectious diseases, delayed development and death in early infancy. Every year 20.6 million children of low birth weight are born. These
children are in special risk for postnatal growth restriction,
infectious diseases, delayed development and death in early infancy.4 million children die in the first month of their lives every year, out of which 27% (1.08 mil.) are preterm infants. The mortality in this group can be reduced by better care, where adequate nutrition is of special importance. Donor human milk versus milk formulae Nutrition by breast milk is associated with lower incidence of early and late infection and necrotic entrocolitis (NEC), and with better psychomotoric development. The length of stay in hospital is also reduced. Children fed by donor milk have significantly better motor skills by the age of 18 months compared to children fed by commercial formulae, but mental development is not different. Although the growth of children fed by fortified donor milk is slower compared to children fed by formulae in the first years of life, in the age of 7.5-8 years the difference is not significant. Also, the incidence of chronic diseases, such as cardiovascular diseases and diabetes is reduced. In the 21st century human donor milk banks have flourished again  This is because human milk contains factors that cannot be replicated in any artificial milk formula, despite constant improvements of their quality. By providing stable source of breast milk, milk banks support breast feeding. Organizing milk banks It consists of: • Motivating voluntary donors • Getting medical history of donors • Medical testing of donors • Training for milk expressing and storage domestic environment • Collection and labeling of milk • Thermal processing (pasteurization and freezing) • Bacteriological testing of milk • Milk distribution Mothers that can be donors: • If they are healthy • If they consent to testing • If they are not taking any drugs or medical supplements Mothers that can not be donors: • If the blood tests are positive for either: HIV, CMV, HTLV, hepatitis B or C, syphilis • If they are in a risk for HIV infection • If they take drugs, medical supplements or narcotics • If they smoke • If they were organ recipients ore have received blood transfusion in the last 12 months • If they drink 2 or more glasses of alcoholic beverages a day Testing of milk donors is performed before the beginning of donations and periodically every 3 months during donation. Training donors for expressing
milk
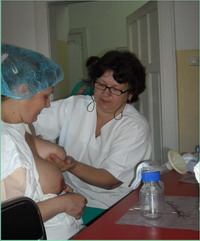 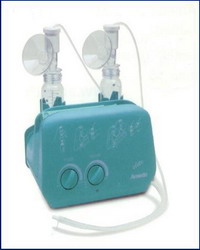
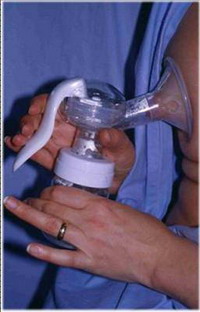 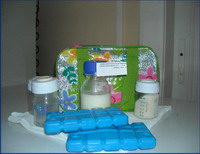 Collection and labeling of milk 
 
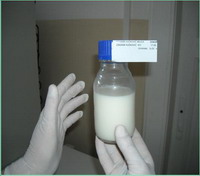 Thermal processing HOLDER PASTEURIZTION 62°C 30’  Freezing and continuous temperature monitoring 
 Analysis of composition and fortification of milk  Serbia In Institute of Neonatology 215 nursing mothers were hospitalized in 2009: • 95 from Belgrade • 113 from other regions of Serbia • 7 from Republic of Srpska (Bosnia and Herzegovina) Lactation was maintained by 76 (35.2%) mothers and they breast fed from 2.5 to 12 months or more. More then 2230 liters of milk were collected. Challenges for first Serbian human milk bank • Recognition by the European Milk Banking Association (EMBA). • Establishment of national guidelines for milk banking. 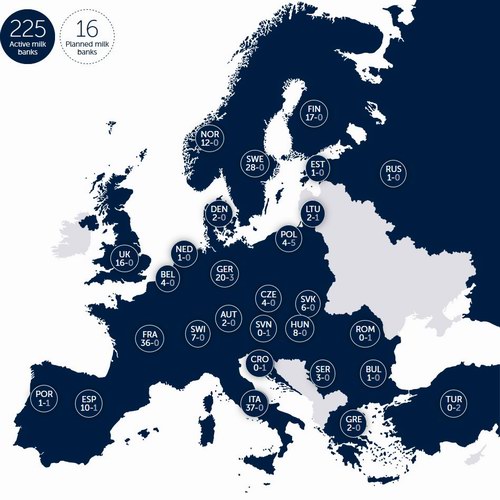 |